50% OFF frames with purchase of lenses.
*Restrictions apply. Click here for details.
Diabetic Retinopathy Screening & Treatments at Clarkson Eyecare
Anyone with diabetes is at risk for developing diabetic retinopathy, an eye condition that damages the retina and can cause vision impairment. The longer you live with diabetes, the more likely it is that you will experience complications from this disease. The retina allows your vision to function correctly. It is a light-sensitive structure on the inner back wall of the eye. When light enters your eye, an image of what is in your field of vision appears on the retina. It transmits these light signals through the optic nerve to the brain, which then translates them into images that your brain can understand.
A network of tiny blood vessels nurture the retina, allowing it to function properly. However, when a diabetic has uncontrolled blood pressure or blood sugar levels, small blood vessels throughout the body may be damaged, including the vessels within the eye. If the retina does not receive enough blood flow, the decline in its function can lead to vision loss. In addition, enlarged or weakened blood vessels can leak small amounts of blood into the eye, blocking your vision. In more advanced cases, abnormal blood vessels can form within the eye, causing additional fluid leakage as well as the formation of scar tissue, which can result in significant vision loss or even permanent blindness.
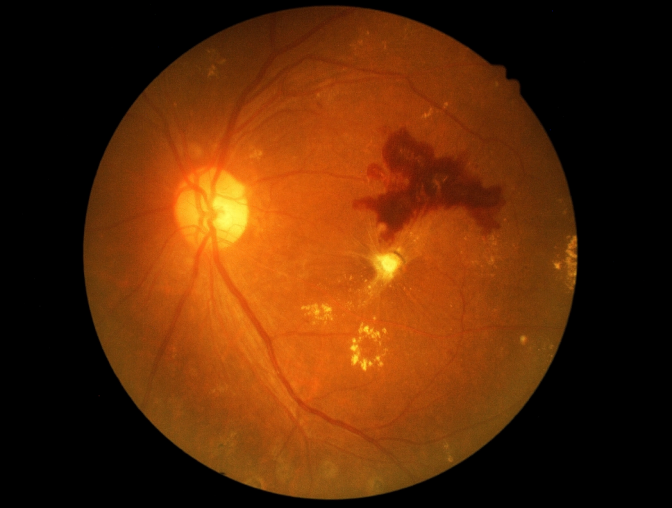
What Are Symptoms of Diabetic Retinopathy?
At first, people who develop diabetic retinopathy may not notice any vision changes because the symptoms are silent in the condition's early stages. When diabetic retinopathy becomes more advanced, it may affect vision in a number of ways:
Your vision may appear blurry
You may notice floaters in your field of vision
Your night vision may worsen, or you may begin to see colors less vividly
You may see dark spots or unexpected blank areas within your field of vision
If you have diabetes and notice any of these vision problems, call your eye doctor for an appointment to assess your eye health.

How Is Diabetic Retinopathy Diagnosed by Eye Doctors?
An eye doctor can assess your retinal health during a comprehensive eye exam. They will most likely dilate your pupils with special eye drops to better examine the inner structures of your eyes.
The eye doctor may also perform a test known as optical coherence tomography, which takes images of the retina to assess its thickness, which may indicate eye diseases related to diabetes.
Another test that may be administered is fluorescein angiography. This procedure helps the eye doctor view the blood vessels in your retina. During a fluorescein angiography, the doctor will inject dye into your arm, which travels through blood vessels to your eyes. The dye appears bright yellow, making it easier for the doctor to view the activity of the tiny blood vessels. Using a specialized camera, the doctor takes images of your eyes to see if the blood vessel activity shows signs of diabetic retinopathy.

What Are the Treatments for Diabetic Retinopathy?
In early stages of the disease, managing your diabetes may be enough to prevent the progression of diabetic retinopathy. However, it is important to see your eye doctor regularly for dilated eye exams to monitor the eye condition for signs of change.
When diabetic retinopathy begins to impair your vision, preventive treatment may not be sufficient. At this stage, more advanced diabetic retinopathy treatment may be critical to preserve your remaining vision. A medication known as anti-VEGF therapy can be injected into the eye after it is numbed and can stop blood vessels from leaking within the eye. Laser treatments can be utilized to seal leaky blood vessels or minimize the presence of abnormal blood vessels. If scar tissue or blood builds inside the eye, it can be removed during surgery to temporarily improve vision.

How Can People with Diabetes Prevent Eye Conditions?
After you've been diagnosed with diabetes, it is imperative that you take any medication prescribed by your doctor to help keep your blood pressure and blood sugar levels in a healthy range. See an eye doctor at least once a year for a dilated eye exam to keep tabs on your eye health, allowing them to catch the early stages of diabetic retinopathy before your vision is permanently damaged.
Good nutrition and regular physical activity can help to keep your blood sugar levels in a healthy range for the prevention of eye conditions. Eating a healthy diet and getting regular exercise can also lower your risk of diabetic retinopathy or can prevent existing retinopathy from developing into later stages.
Diabetic retinopathy can lead to significant vision loss and permanent blindness, but these complications of the disease can be prevented by practicing self-care and following the advice of your eye doctor.